Research
 Our program attracts the best and the brightest research trainees from around the United States and the world to work in more than 2 dozen research programs that investigate all aspects of pulmonary and allergy biology and disease. We participate in virtually every nationally funded pulmonary disease research network and have well-funded and highly productive research programs at each of 5 UCSF campuses. Our faculty also play important roles in many of the premiere inter-disciplinary research and training programs at UCSF, including the Cardiovascular Research Institute, the Helen Diller Family Comprehensive Cancer Center, the Center for Global Health Sciences, the Immunology Program, the Biomedical Sciences Graduate Program, the Program in Biological Sciences and the Program in Human Genetics. Division faculty members also play leadership roles in the American Thoracic Society (5 former Presidents) and in advising the National Institutes of Health and the World Health Organization. Research initiated in our division has already been translated into new therapies for asthma, acute lung injury, pulmonary fibrosis and tuberculosis.
Our program attracts the best and the brightest research trainees from around the United States and the world to work in more than 2 dozen research programs that investigate all aspects of pulmonary and allergy biology and disease. We participate in virtually every nationally funded pulmonary disease research network and have well-funded and highly productive research programs at each of 5 UCSF campuses. Our faculty also play important roles in many of the premiere inter-disciplinary research and training programs at UCSF, including the Cardiovascular Research Institute, the Helen Diller Family Comprehensive Cancer Center, the Center for Global Health Sciences, the Immunology Program, the Biomedical Sciences Graduate Program, the Program in Biological Sciences and the Program in Human Genetics. Division faculty members also play leadership roles in the American Thoracic Society (5 former Presidents) and in advising the National Institutes of Health and the World Health Organization. Research initiated in our division has already been translated into new therapies for asthma, acute lung injury, pulmonary fibrosis and tuberculosis.
UCSF has long been a world leader in basic, clinical and translational pulmonary and critical care research.
Basic Biology
UCSF is one of the leaders in basic lung biology, exploring fundamental principles that govern immunology, stem cell biology, matrix biology, developmental biology, genetics, and cell biology in the lung. Our labs span across multiple campuses, including Parnassus Heights, Mission Bay, ZSFG, and SFVAMC
Airwary Disease/Allergy/Environmental Disease
UCSF has a long history of research in allergy and asthma and especially in mechanisms of airway inflammation in asthma. Over the past 50 years, multiple faculty members at UCSF have contributed importantly to current knowledge of the specific cells and mediators that drive allergic inflammation and asthma. Seminal discoveries at UCSF have provided rationale for the treatment of asthma with inhaled anticholinergic drugs and anti-inflammatory drugs such as corticosteroids, leukotriene receptor antagonists, and anti-cytokine therapies (especially anti IL13). UCSF has also been a leader in identifying molecular subtypes of asthma and in developing biomarkers for specific asthma subtypes.
Interstitial Lung Disease
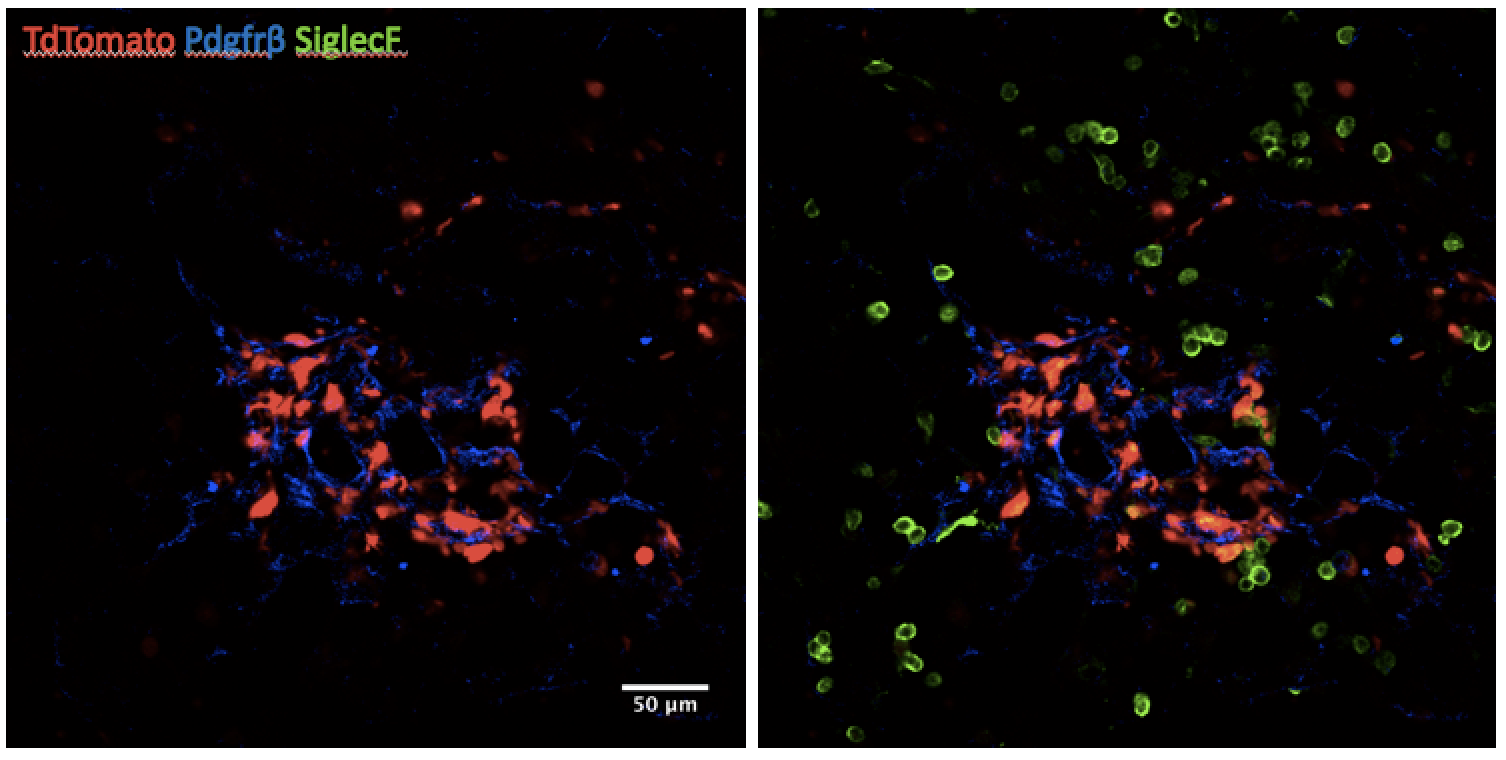
UCSF has an active research program conducting both clinical and basic research in the pathogenesis of lung fibrosis. Through the generosity of our patients, who collaborate with our world-class physician scientists, we have developed a better understanding of the fundamental, cellular and molecular mechanisms of interstitial lung disease.
LUNG TRANSPLANTATION
Over the last three decades, lung transplantation has grown exponentially. Today, it aims to improve survival and health-related quality of life for patients suffering from advanced non-malignant lung diseases. Driven by these two overarching aims, our group of investigators at UCSF are focused on advancing the practice of lung transplantation and understanding the mechanisms driving key clinical outcomes including chronic allograft rejection and malignancies after transplant.
Critical Care/Lung Injury
Critical Care Medicine research at UCSF includes Acute Lung Injury and Sepsis. Both are a major focus for basic and clinical research. The research opportunities include molecular, cell and organ based studies as well as patient based research. In addition, there is an opportunity to participate in phase 2 and 3 clinical trials. UCSF has a long tradition of NIH supported research in sepsis and acute lung injury with a history of being one of the major national and international leaders in both basic and clinical research and pivotal clinical trials.
Global Health
Worldwide, lung conditions account for four of the top 10 causes of death. In addition to chronic obstructive pulmonary disease (COPD) and lung cancer, pneumonia (#4) and tuberculosis (#10) are leading causes of death. Faculty in our division are active both locally and globally in improving the clinical care and advancing our knowledge of lung infections
Cancer

UCSF is a regional, national, and international referral center for lung cancer treatment. Research in lung cancer takes place in the Pulmonary Division, Medical Oncology, the Department of Surgery, the Helen Diller Comprehensive Cancer Center and ImmunoX. New initiatives related to Immuno-oncology including efforts to profile the immune environment in lung cancer are ongoing across these departments given the great promise of immunotherapy for lung cancer.
Sleep
Sleep research at UCSF is closely integrated with the UCSF Sleep Disorders Center, an active clinical program with an 8-bed sleep laboratory for overnight polysomnography.
